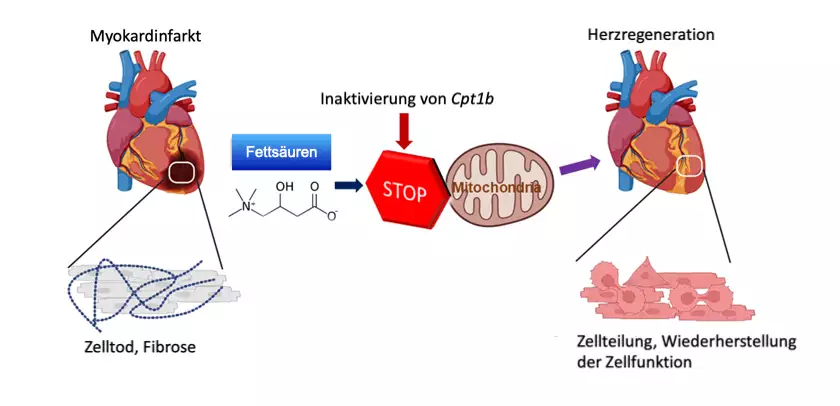
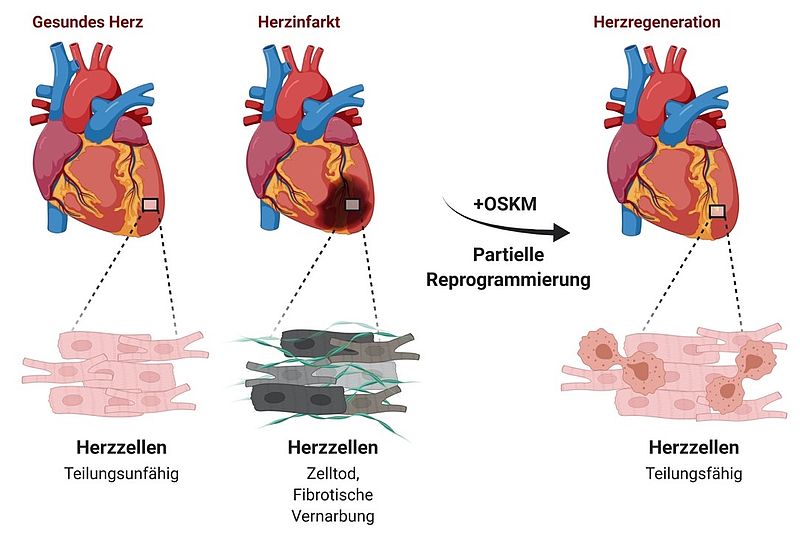
Shortly after birth, the human heart largely loses its ability to repair itself in case of damage. Injuries or diseases of the heart muscle therefore lead to permanent damage and a restriction of the heart function. One of the reasons why the heart muscle loses its ability to regenerate is that the heart muscle cells can no longer divide after birth. This is accompanied by a fundamental change in the energy metabolism of the heart cells: Instead of obtaining energy from sugars, which is called glycolysis, the heart muscle cells now obtain most of their energy from fats. This form of energy production is called fatty acid oxidation.
The research group of Thomas Braun, DZHK-PI and Director at the Max Planck Institute for Heart and Lung Research in Bad Nauheim, has started looking for new methods to promote the regeneration of the heart, starting with energy production: "We know that animal species that can regenerate their hearts, primarily use sugar and glycolysis as fuel for the heart muscle cells. The human heart also uses mainly glycolysis in early stages of development, but then switches to fatty acid oxidation, as this can produce more energy," explain Xiang Li and Xuejun Yuan, authors of the study. "With the switch in energy production after birth, the activity of many genes changes and cell division activity is lost. Individual metabolites from energy production also have important functions for the activity of enzymes that regulate gene activities. We therefore hoped to trigger changes in gene activities by reprogramming the energy metabolism in order to switch cell division ability back on in cardiac muscle cells."
Inactivated gene for fatty acid oxidation
To do this, the Max Planck researchers first inactivated a certain gene called Cpt1b in mice, which is essential for fatty acid oxidation. "We then observed that hearts in these mice started to grow again," Li explains. Over the course of the experiment, the cell numbers in the hearts of these mice nearly doubled.
In the next step, the Bad Nauheim researchers triggered heart attacks in mice in which Cpt1b was switched off. In the chosen approach, a phase of missing blood flow to the heart is followed by a reperfusion phase in which the heart is flushed with oxygen-rich blood again. "This model is comparable to a heart patient whose heart is treated with the insertion of a stent due to an occlusion of the coronary vessels," Yuan explains. The effect was impressive: otherwise usual scars in the heart muscle were hardly noticeable after weeks and the contractility in animals without Cpt1b almost returned to the level before the infarction.
Regenerative capacity returns
In further investigations, the scientists were able to decipher the underlying mechanism: "In heart muscle cells of the mice with the inactivated gene, we found a twenty-fold increased level of alpha-ketoglutarate. The high level of this metabolite leads to a significant increase in the activity of the enzyme KDM5," Braun explains. This enzyme is a so-called histone demethylase, which removes methyl groups from histones and thus reduces the activity of various genes. Through the change in gene activity, heart muscle cells become more immature and thus regain the ability to regenerate.
Braun sees the study as a real breakthrough: "By reprogramming the metabolism, we double the number of heart muscle cells and after an infarction, heart function is almost completely restored." In addition, it is in principle possible to pharmacologically block the activity of the enzyme CPT1B - the gene product of Cpt1b. The development of an inhibitor that can influence the activity of the enzyme CPT1B is the next step on the way to developing a therapy that can eventually be used in humans. However, Yuan and Braun emphasise: "We still have a long way to go before reliable treatments in humans become possible. The implementation of new findings from basic research is long and expensive and is often accompanied by many unexpected problems. Nevertheless, we are confident that we will be able to therapeutically stimulate the regenerative capacity of the heart in the future.
Original publication: Inhibition of fatty acid oxidation enables heart regeneration in adult mice (Li et al., Nature, 2023)
Scientific contact: Prof. Dr. Dr. habil. Thomas Braun, Max-Planck-Institute for Heart and Lung Research, Bad Nauheim, thomas.braun(at)mpi-bn.mpg.de
Source: MPG press release