Coronary heart disease is the leading cause of death in Germany. It is caused by calcium deposits in the coronary arteries, which supply the heart muscle with oxygen-rich blood. If this calcification causes blockages, the blood flow to the heart muscle is reduced. One of the main treatments for CHD is percutaneous coronary intervention (PCI): A tube-shaped support, known as a stent, is inserted into the vessel via a heart catheter to keep it permanently open. The precise and safe placement of this stent is crucial for the prevention of complications and the long-term success of the treatment.
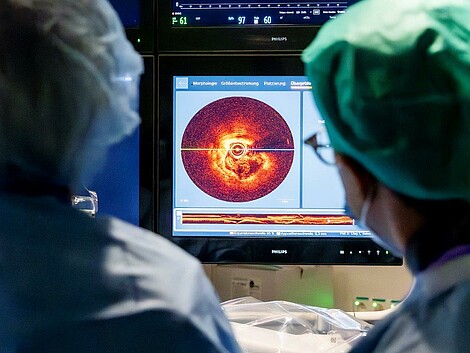
Angiography is the established imaging technique used to monitor the procedure: This involves injecting a contrast agent into the blood vessels so that they become visible on an x-ray of the heart during the procedure. Doctors also have access to optical coherence tomography (OCT), a laser-based imaging technique. It produces high-resolution images of the inner walls of blood vessels and provides a clear picture of blockages and damage.
The multi-centre ILUMIEN IV study, published in the New England Journal of Medicine and presented at the European Congress of Cardiology in Amsterdam, investigated the additional benefit of this procedure. With 2487 patients enrolled in 18 countries, it is the largest study to date on this topic worldwide. Prof. Dr. med. Ulf Landmesser, Deputy Medical Director of the DHZC and Head of the DHZC Clinic for Cardiology, Angiology and Intensive Care Medicine at the Benjamin Franklin Campus, is one of the two principal investigators.
All enrolled patients were considered "high risk" because of their diabetes or the severity of their coronary heart disease. Approximately half of the patients underwent PCI using OCT or angiography. The analysis showed that the cross-sectional area of the stents placed with the help of OCT was larger and that - in simple terms - a "better stent opening" was achieved in the treated coronary artery. A large stent area is therefore an important criterion for the long-term success of the treatment.
Accordingly, there were significantly fewer complications during OCT-guided PCI. In particular, dangerous stent thrombosis and vessel occlusion due to thrombosis of the stent support occurred significantly less frequently in the OCT group. In the long-term results, however, the study data did not show any significant difference between the treatment groups with regard to the need for repeat treatment of the treated vessel.
However, the authors point out that this long-term result could be influenced by the COVID pandemic: Patients' fear of hospitalisation and the limited resources of the healthcare system during the pandemic may have reduced the number of repeat treatments. Despite this limitation, Ulf Landmesser sees the study as a sustainable contribution to the further improvement of PCI with high clinical relevance: "Our results, together with the current meta-analysis, underline the efficiency and safety of OCT technology and provide treating colleagues worldwide with a valid data-based basis for the choice of imaging in the coronary artery".
Original publication: https://www.nejm.org/doi/10.1056/NEJMoa2305861
Scientific Contact: Prof. Dr. Ulf Landmesser, Director of the Clinic for Cardiology, Angiology and Intensive Care, Charité Berlin
Source: DHZC press release